29 May 2023
Food allergens are proteins found in foods that can cause adverse reactions in allergic individuals. The presence of these allergens can be a serious health concern for some people and can cause fatal allergic reactions.
Food allergen testing is a key aspect of food safety, both for protecting allergic consumers and for protecting the reputation of the manufacturer. It can be critical in providing evidence for contamination investigations, substantiation of free-from claims, or in decision making for precautionary allergen labelling. There are a wide variety of testing methods available to look for the presence of allergens in food, the most appropriate method to use is dependent on many factors, including the allergen in question as well as the nature of the food product itself. Each method has its own set of advantages and disadvantages, and biological tests are prone to false negative and false positive results, so making the right choice for your testing strategy is essential.

Two of the most recommended and performed methods for allergen testing are ELISA (Enzyme-linked Immunosorbent Assay) and PCR (Polymerase Chain Reaction).
ELISA is a quantitative test that targets specific proteins, which can make the testing more clinically relevant, as it is the protein which causes the reaction in allergic consumers. The results from an ELISA analysis are usually quantitative and can be reported or converted into a protein which typically makes this the first choice for allergen testing. Having a quantitative result expressed in protein can be important, especially if you are using reference dose calculations and relating the result back to consumer risk or performing cleaning validations where quantitative results are recommended.
PCR is a DNA technique, which targets a specific sequence of DNA unique to the food containing the allergen. PCR tests tend to be qualitative. The results obtained cannot easily be converted into protein, and the presence or absence of DNA does not necessarily prove presence or absence of protein. Therefore, PCR is not typically recommended where a suitable ELISA test for allergens is available. Some foods however can cause adverse matrix interferences with ELISA tests and the proteins can be degraded or altered during food processing, which may cause them to be more difficult (or in some cases not possible) to detect with ELISA. In these cases, a PCR test may be more suitable.
There are other techniques that can be used, for example LC-MS/MS (Liquid Chromatography Tandem Mass Spectrometry) which digests proteins into peptides to detect. This technique is a highly sensitive, quantitative analysis; however, it is hard to translate the result into allergen protein. Currently there are no standardised allergen methods for this technique, which can lead to variability of results. There is also a high cost associated with the analysis. Therefore, at this time LC-MS/MS is typically only used when ELISA or PCR is not suitable due to complex matrixes or highly processed contaminants. Sulphites cannot be detected using the above methods and instead requires a distillation or titration method to isolate and capture the sulphur dioxide. The selected sulphite method will depend on the sample type and can be used for food samples and rinse waters.
Foods are complex matrices and biological tests can be prone to matrix interferences, causing adverse reactions in the testing and impacting the validity of the test. Hence, it is important to collect evidence that the right test has been chosen for you and avoid potential false positive or false negative results. This can be done through performing extra competencies like spike recovery tests, cross-reactivity checks and analysing positive controls (explained in more detail below).
A false positive result occurs where the test detects the allergen and reports a detected result, when no allergen was present in the sample. This could be a risk to your business and result in an unnecessary recall or investigation.
A false negative result occurs where the test could not detect the allergen and reports a not detected result, despite an allergen being present in the sample. This could be a risk to both the consumer and the business as product will be released and an allergic consumer could have a reaction, potentially leading to a public recall.
Spike recovery checks are an important part of mitigating against potential false results, as they provide evidence that the test you have chosen is suitable for your sample type. A spike recovery check involves adding a known quantity of the allergen to an aliquot of your sample, analysing it, and then comparing the result obtained against the known quantity of allergen added. The laboratory can determine if the result is within the expected range and whether the ingredients are adversely reacting to the test, based on the percentage of allergen the analysis was able to recover.
Cross-reactivity occurs when the test mistakenly detects something as the allergen it was looking for. Usually cross-reactivity is caused by something that is biologically similar to the allergen, e.g. a similar shaped protein or sequence of DNA. For example, all mustard ELISA kits cross-react with rapeseed and other seeds from the Brassica genus, and walnut PCR tests often cross-react with pecan. When there is a detected result that is unexpected from the analysis, cross-reactivity checks can be completed by the laboratory to rule out a potential false positive result.
Positive control testing can be a useful tool if you know your contaminant. This is where a product or ingredient that contains the allergen of concern is sent in for testing to prove that the test can detect the allergen when it is supposed to be there. If the test cannot detect the protein when it is supposed to be there as a deliberate ingredient, for example due to processing or interference, then the test will not detect the protein when it is there unintentionally in small quantities.
Factory based tests, like RLFD (Rapid Lateral Flow Devices), can be useful as a verification tool as they are quick and easy to use. They are typically designed for rinse waters and environmental swabs, as the extraction procedures are not exhaustive and often quite rudimentary, and a complex matrix like food can easily cause interferences. It is important when using RLFDs that they are validated, as the advertised detection limits can vary depending on the source of contaminant. For example, the detection limit for a milk RLFD may be based on liquid milk but the detection limit may be different if the contaminant is different, e.g., cheese or whey.
There are many challenges when it comes to food allergen testing and it is important to pick the right testing method based on your sample matrix and contaminant. Therefore, it is important that you choose a laboratory that can help you understand, navigate, and mitigate these challenges.
When looking for a laboratory, consider whether they are independently accredited against BS EN ISO/IEC 17025, not just for their laboratory but ideally for the specific test method as well. Will they perform extra validations, such as spike recovery testing and cross-reactivity checks? Consider how good their communication is with you, are they able to help you choose the appropriate test for your sample and can they help you understand and interpret the results? You will want them to have good experience and expertise in food allergen testing as well as a good understanding and up-to-date knowledge of the food industry.
Most of the major allergenic food proteins are relatively stable and the protein structure is not significantly altered or destroyed under normal commercial food processing conditions, such as heat treatment, canning, and freeze-drying. However, processing the protein may change the shape enough for the analytical test not to be able to effectively detect it, potentially leading to a false negative result. Although the test may not be designed to recognise the altered protein, we know processing can, in some cases, make the protein less or even more allergenic to the allergic consumer meaning they are more sensitive to the protein and more likely to have a reaction.
When egg white is denatured in its cooked form, a significant number of the ELISA tests available are not able to detect these denatured proteins effectively.

Information regarding the tests not being designed to detect cooked egg is widely published in literature, however we often see instances where the inappropriate test, that does not detect cooked egg effectively, is used when cooked egg is the contaminant.
In one instance, the manufacturer of egg containing and non-egg containing products had been using a UKAS accredited laboratory to test their finished product for egg, as well as using RLFDs as a verification tool, which they had not validated. The manufacturer had been obtaining not-detected results for several years from both analyses, however when a retailer commissioned RSSL to complete some surveillance testing, we discovered that egg was in fact present in their non-egg containing product. An investigation was undertaken by RSSL, the manufacturer, and the retailer and it was determined that the egg-containing product was a cooked form of egg and the ELISA and RLFD test the manufacturer was using were not suitable for detecting protein from cooked egg.
To collect evidence that the ELISA test they were using was not suitable, the manufacturer commissioned some testing of their egg-containing product, with a theoretical protein content of approximately 6,000 ppm egg protein, to three different UKAS accredited laboratories: RSSL, the manufacturer’s existing laboratory and a third laboratory (previously uninvolved in the incident). The results are shown below:
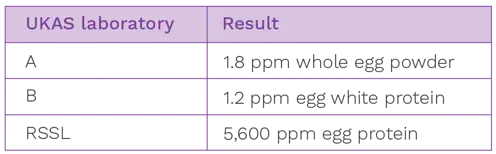
This testing highlighted that the two egg ELISA tests that laboratory A and B were using were not suitable for the manufacturer’s contaminant, as they were not effective at detecting proteins from cooked egg. Had positive control testing been completed at the start of the manufacturer’s testing they would have known this and chosen a more appropriate test. This shows the importance of performing the extra validations listed above as well as partnering with a laboratory that can help mitigate the challenges that come with food allergen testing.
In conclusion, food allergen testing is critical when it comes to food safety and can help to keep allergic consumers safe. There are a wide variety of testing methods available each with different challenges. The most suitable method to use for testing can change depending on the contaminant, the sample type, and the target allergen. Partnering with a good laboratory is key to navigating the different risks surrounding allergen testing and choosing the most appropriate test for you.
Our state-of-the-art UKAS accredited laboratory and expert allergen team use analytical techniques to detect and quantify allergens in a wide range of food products. We offer a range of testing methods, including ELISA and PCR, and can provide results quickly and efficiently. We can also provide guidance on allergen risk assessments, develop and validate allergen detection methods and provide allergen training to ensure the safety and compliance of your products. Click through below to find our more our contact us via the enquiry form below.